0 Comments
We are delighted to share that Fortify Health has received a GiveWell Incubation Grant of ~$1,000,000. This grant will provide the organisation with two years of funding for operations in Maharashtra and West Bengal, from implementation to expanding the team. In Fortify Health’s third year of existence (from mid-2019), the focus is on scaling up implementation.
June 2019 to May 2020: First year of GiveWell Incubation Grant Over the first year of GiveWell’s 2-year grant, the funding will be directed primarily towards expanding open market wheat flour fortification and building strong partnerships in our two focus states: Maharashtra and West Bengal. Our goals for May 2020 are:
June 2020 to May 2021: Second year of GiveWell Incubation Grant The second year of funds will be used to continue the mill partnerships and involvement in government programmes achieved in the first year, and to maintain our team. In order to keep expanding in Year 2, we will need to apply for further funding from GiveWell or other sources. Possibility of further expansion and strategy direction are also dependent on new research that may alter effectiveness or cost-effectiveness estimates of fortification. In early 2020, we will refine our strategy for the trajectory of Fortify Health’s operations. Thank you The receipt of these funds is a testament to the work of our team over the past two years, who have been driven, dedicated and collaborative along the journey to this milestone. We would also like to thank each and every individual who has supported and advised us along the way, including but not limited to:
 We couldn't be more excited to welcome Dr. Urmi Bhattacharya in her new role as Country Director to the Fortify Health team. Urmi joins with extensive experience relevant to fortification, management, and monitoring & evaluation. Prior to joining Fortify Health, Urmi was a Research Manager at the Abdul Latif Jameel Poverty Action Lab (J-PAL) South Asia for four years, where she managed six large scale programmes across five states in India, including two fortification studies. She has also served as the Global Head of Monitoring and Evaluation for Uganda and India at STIR Education. Urmi earned her PhD in Economics from Indiana University in 2012 and has since dedicated her passion and skills towards making high quality education and health systems accessible to all people. We’re delighted to announce that over the past few weeks we’ve welcomed on board three new full-time team members. After completing our first ever round of recruitment over the summer months, we’ve hired a Programme Officer, a Partnerships Officer, and a Senior Partnerships Officer. Introducing:  Shweta, Programme Officer Shweta has worked as a Research Associate at JPAL South Asia on Non-Communicable Diseases project. She led the RCT study in Mumbai that assessed the impact of reminder call services on compliance to diabetes treatment among elderly populations. Shweta has also worked with the Overseas Development Institute as a Research Intern, studying perceptions of youth on working in the agricultural sector, and its impact on agriculture in Uganda and Ghana. She has completed MSc in Anthropology and Development from the London School Of Economics.  Muneer, Partnerships Officer Dr. Muneer holds a Master’s in Health Administration from the Tata Institute of Social Sciences, Mumbai and a Bachelor’s in Ayurvedic Medicine and Surgery from Amrita University. Before joining Fortify Health, he was working with Public Health Resource Network in Delhi coordinating the end to end implementation of a nutrition programme in Odisha. His interests include public health, nutrition, anthropology, international politics, history and geography. He is an aficionado of ghazals and Indian classical music.  Shiva, Senior Partnerships Officer Shiva holds a degree in social work from CSRD- Institute of Social Work and Research, Ahmednagar with academic achievement of clearing UGC, NET. He previously worked with STIR Education as a Senior Program Manager, where he was closely associated with ministries and the education department in Delhi, Maharashtra and Tamil Nadu. He was a also Gandhi Fellow, working on School Leadership Development with the Govt. schools in Gujarat. His interest lies with evidence-based interventions, government partnerships, and policy intervention. Fortify Health is excited to announce that we have received a GiveWell Incubation Grant. This will allow us to continue setting up a micronutrient initiative in India over the next year. GiveWell has recommended a grant to fully fund our budget of $295,217 and has published their review of Fortify Health on their website. Our intervention takes a two-tiered approach to improving fortification in India. Firstly, we will work with industrial flour millers to facilitate addition of iron, folic acid, and vitamin B12 to wheat flour, offering immediate measures to prevent anemia and neural tube defects (NTDs). Simultaneously (and secondly), we will take a longer-term approach by supporting a state government to develop sound fortification standards, implement an effective monitoring and evaluation system, and progress towards a fortification mandate. Our brief plans for the next year will be to:
Once fortification is underway, we will focus more on quality assurance, and monitoring and evaluation of fortification programmes. In January, Fortify Health’s founding team conducted a visit to India. Our aim was to learn about project opportunities to contribute to ongoing efforts in food fortification. We learned critical information about the food fortification landscape and norms in India, including challenges and progress, as well as identifying specific programmes we could start up. To understand the complexities of fortification in India, it is important to be aware of the Indian government’s safety net programmes and food industry norms. Read our background notes to learn more. We spoke with key players in fortification, meeting with the government’s Food Fortification Resource Centre and a range of NGOs working in flour or rice fortification: Global Alliance for Improved Nutrition (GAIN), PATH, Food Fortification Initiative, Nutrition International and World Food Programme. We have published summary notes from key conversations, which you can find below: Food Fortification Resource Centre PATH Global Alliance for Improved Nutrition Food Fortification Initiative Nutrition International World Food Programme From these conversations and from our own models and cost effectiveness analysis, we have developed several project proposals for fortification projects we believe to be highly impactful. These will be online and publicly accessible soon. This post provides an update on our progress and explains our decision to explore opportunities to add value to iron and folic acid fortification in India. Having extensively reviewed the academic literature and NGO reports, and having spoken to experts in the field who strongly encouraged us to develop this project even as non-experts, we set out to understand where in the world a new fortification initiative might have the most impact. The approach to our evaluation was driven by data and expert guidance.
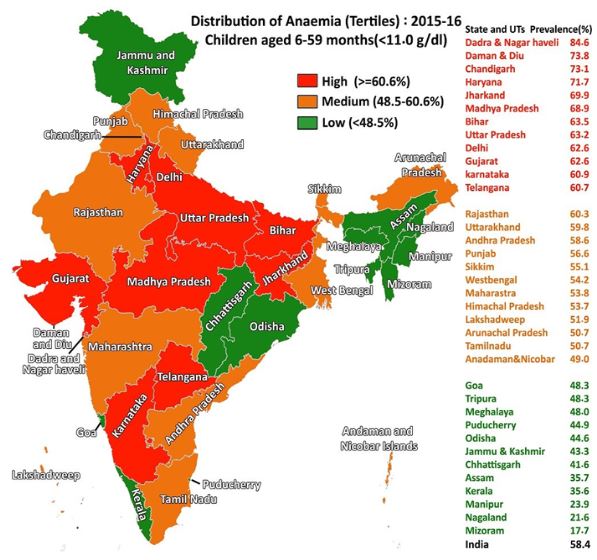
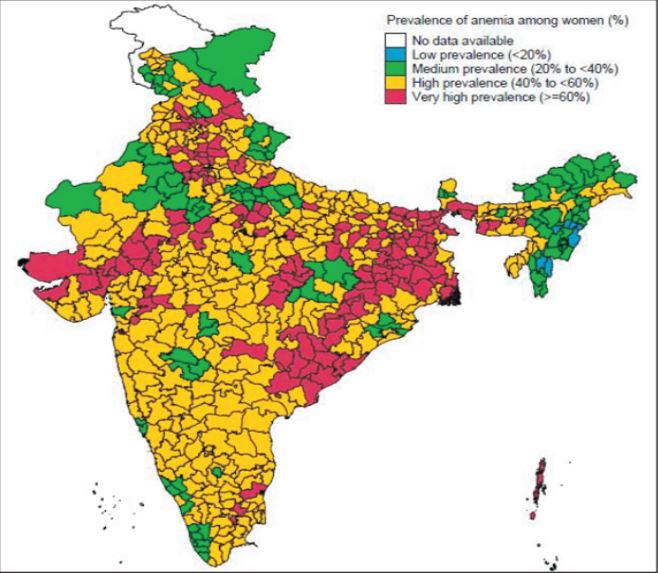
For an overview of why we began working on iron and folic acid fortification and for background information about iron deficiency anemia and neural tube defects, please see our previous post. We began our evaluation with country-level analysis of available data, including disease burden, potential intervention scale, status quo fortification gap of centralized mills, and potential risks (contraindications). These were complemented by estimated parameters for more subjective factors, including conflict, crowdedness, language barriers, and miscellaneous positive factors. These scores were standardized and weighted to compute a composite score for each country. Data are available in this spreadsheet. Disclaimer These scores and the suggested weights are certainly not a literal indication of the importance of further fortification efforts in the countries evaluated. While this framework was useful in guiding our location selection, we do not claim that its guidance is absolute nor do we claim that fortification (or access to plentiful nutritious food and good health, for that matter) is any less important in locations with lesser scores. Consider this spreadsheet as a visualization of various factors relevant to determining with limited information where our new initiative might be expected to have the highest potential impact. Selection criteria Disease burden was modeled as the combined DALY rate of iron deficiency anemia and neural tube defects. Potential intervention scale was modeled as the log of the country’s population. As such, larger countries with greater potential scale were nonlinearly compared (e.g. India’s population of approximately 1.3 billion was scored approximately twice as high as Sudan’s population of approximately 40 million). This transformation was deemed reasonably aligned with assumptions of potential scale (e.g. the feasibility of working within one state in India compared to at a national level in a smaller country). The status quo fortification gap of centralized mills was calculated given data aggregated by the Food Fortification Initiative on staple food consumption, centralization of milling of rice, wheat, and corn, and the amount of that staple that is currently fortified. As such, an estimate of the the centrally produced fortifiable food not currently fortified was used in comparison. The primary potential risk factor (contraindication) considered was the burden of malaria, expressed by national DALY rate. Existing data and meta analysis suggest that iron supplementation programs are associated with increased risk of malaria contraction in high burden regions lacking malaria services. Iron supplementation differs from iron fortification: supplementation involves consumption of high-dose iron tablets at varied frequency (daily to biannually, depending on program) whereas fortification involves consumption of low-dose trace amounts of iron consumed regularly through fortified staple foods. To our knowledge and informed by expert consultation, data on the impact of fortification on malaria risk is not currently available. Even so, several programs are currently underway under the assumption that the low dose of fortification would not carry the same risk. We believe this is an area of worthwhile exploration and would be happy to work with a health economist or statistician to analyze existing data to produce informative evidence. Given the present uncertainty, we included malaria risk as a contraindicating factor in our location selection. Political feasibility, the presence of ongoing war or political instability, was subjectively rated to reflect both the feasibility of working with government approval or collaboration, the endurance of implemented programs, and safety establishing projects. Language barriers were considered to reflect our confidence that we could build partnerships with local organizations and governments. Countries where English is spoken (our native language) scored higher than countries where Spanish, German, or French is spoken (our non-native languages), which scored higher than countries where none of the four languages is spoken. Crowdedness, the presence of existing actors already doing (or planning to do) work similar to our aims, was assessed by reviewing the governmental and NGO efforts currently underway in countries scoring highest on the aforementioned factors. A subjective score was assigned to each evaluated country. Miscellaneous positive factors included existing relationships with potential partners or influential people. Selecting India Considering these factors, India emerged the most promising location to explore specific opportunities for our work. By comparison to other top candidates, India scored slightly to moderately lower on disease burden, higher on potential intervention scale, higher on status quo fortification gap, substantially lower on malaria risk, slightly lower on political feasibility (the average scores of top locations was heavily skewed by Bhutan), higher on crowdedness, lower on language barriers, and higher on miscellaneous factors. Put another way, reasons to work in India compared with other top candidates included potential intervention scale, status quo fortification gap, low malaria risk, lower language barriers, and positive miscellaneous factors, even though other top candidates had somewhat higher disease burdens and appeared less crowded. Across India, 38.3 percent of the population suffers from iron deficiency anemia (compared to 2.3 percent in the US). Anemia affects 55.3 percent of women and 69.5 percent of children in India considering all causes (including anemia resulting from iron deficiency, intestinal worms, etc.). Expert views Having connected with several experts working in the field, we have overwhelmingly received encouraging responses to our initiative (and have been grateful for pushback, as well). Despite several actors’ efforts on micronutrient fortification in India, it became clear from conversations with organizations working on fortification in India that there is plenty of room for further focus. Anemia is a substantial problem in India and existing interventions are sparsely implemented. Overview
We’re engaging in an exciting entrepreneurship experiment: can a new organization with an effective altruism aligned approach effectively reduce the burden of iron deficiency anemia and neural tube defects? The burden is so large that we hypothesize that there exist opportunities for impact beyond already excellent work being done by major organizations. We have begun to develop relevant expertise and curate potential strategies for intervention. We are now consulting with experts to deepen our expertise and build partnerships, as well as narrowing down potential locations in which to focus our work. We hope to develop a GiveWell-worthy charity that can exceptionally effectively put donations to work in improving the lives of vulnerable people. We believe that despite the challenges to achieving this ambitious goal, this initiative is worth our efforts. It provides great career capital and learning opportunities for us, and we believe this project will have valuable lessons for the effective altruism (EA) movement. We are grateful for the opportunity to work on this potentially high-impact and exciting project. The problem Anemia and neural tube defects are widespread, preventable health problems that primarily lead to the suffering of women and children. Poverty predisposes people to anemia and neural tube defects for a variety of reasons, including inadequate nutrition, weak health systems, infectious/parasitic disease, and limited access to fortified foods. Iron deficiency anemia (IDA) occurs when the body does not have enough iron to produce hemoglobin and cannot carry sufficient levels of oxygen around the body. IDA is responsible for roughly half of the 2.36 billion cases of anemia globally, and accounts for four percent of all years lived with disability. Anemia can cause chronic tiredness/fatigue, impaired cognitive development in children, low moods and low productivity in adults, and even increase risk for depressive symptoms and heart disease. Neural tube defects (NTDs) are developmental abnormalities affecting the spine, spinal cord, and brain, largely due to folic acid deficiency within the first month of pregnancy. NTDs account for over five million DALYs and over 40 thousand deaths annually. A response Fortification of staple foods with iron and folic acid is an evidence based strategy to reduce the burden of these diseases. IDA and NTDs account for widespread illness and their prevention is evidence-based and cost-effective. An organization transparently and successfully facilitating fortification would align well with Givewell’s criteria for exceptionally effective organizations, and we’ve set out to try to develop such an organization. Charity Science is incubating this initiative. According to their rigorous evaluation, iron and folic acid fortification is among the top causes that could become a GiveWell top charity. Causes were evaluated in terms of cost-effectiveness, scalability, strength of evidence, ease of testing, flexibility, and logistical possibility. Experts in the field, including GiveWell, 80,000 Hours, and Charity Science think charity entrepreneurship is an effective way to make a difference in the world. What we hope to learn Is it possible or realistic for non-expert, effective altruism-aligned individuals to establish a GiveWell-worthy organization from scratch? In the interest of setting up an organization that meets GiveWell’s criteria, we are eager to test the possibility of EAs founding effective charities. Our first steps have been to begin gaining expertise on iron and folic acid fortification, and we will be grateful to the experts willing to share their knowledge with non-experts entering the field. Charity Science: Health, an EA-aligned organization that provides SMS reminders for vaccines, is a good example of an implementation organization that has been developed from scratch by non-experts. This is the only charity startup of its kind that we are aware of and we hope to employ a similar model in building a micronutrient fortification initiative. Are there gaps in the current work focused on IDA and NTDs through staple food fortification that likely won’t be met by other institutions in the near future? At present, one of our priorities is to understand the current global landscape in micronutrient fortification and the different stages involved in the fortification process. By extensive reading and expert consultation, we hope to pinpoint the most neglected areas in the fortification process and we are considering a range of potential strategies (discussed below). As we gain expertise and familiarity with the existing actors, we will prioritize potential locations and strategies. Who are we? Brendan Eappen, Co-Founder, most recently worked with Partners in Health (Socios en Salud) in Peru on the development of their mental health program. Brendan studied Cognitive Neuroscience & Evolutionary Psychology, and Global Health & Health Policy at Harvard College. Nikita Patel, Co-Founder, most recently worked at Malaria Consortium in global health communications, and prior to this completed an internship at the Centre for Effective Altruism. Nikita studied French and German at University of Oxford. Joey Savoie, Mentor and Funder, CEO and Co-Founder of Charity Science (an effective altruism organization based in Vancouver) is providing extensive mentorship and initial funding. Joey directs Charity Science: Health, the first EA-aligned charity startup of its kind. Their project sends text message reminders for vaccinations in India, where only 65 percent of the 20 million children in India receive all recommended vaccinations by age two. Charity Science: Health has been awarded two GiveWell incubation grants. If fortify hEAlth advances beyond its initial stage, we plan to hire industry experts with specific skills and experience relevant to the chosen strategy and location. Progress so far In brief, during our first month, we have:
Potential approaches Our initial research suggests that, despite the attention of several organizations to iron deficiency anemia (IDA) and neural tube defects (NTDs), there may remain many gaps that prevent people from access to iron and folic acid. Several potential approaches may be employed to improve access to these key nutrients and therefore combat IDA and NTDs. Any strategy we implement would be pursued in coordination with local organizations, international organizations, academic experts, and others. We will rigorously evaluate the potential for EA-aligned action consistent with these and other strategies. Here are some intervention approaches we have identified as possibilities:
The above strategies are particularly appealing because of the scale of the potential impact. However, if further investigation proves they are either too crowded or infeasible, our efforts may be most impactful in extending fortification initiatives to communities often outside their reach, such as by:
If you would like to learn more, guide us, or join us, please email us. Especially if you have expertise in this domain, but in any case, we would love to hear from you. |
- About us
- What We Do
- Resources
-
Get Involved
- Donate
-
Jobs
>
- Senior Quality Officer (Pune/Aurangabad)
- Senior Partnerships Officer
- Senior Program Manager
- Associate Director of Monitoring, Evaluation and Research
- Quality Systems Manager
- Senior Monitoring and Evaluation Officer
- Senior Data Officer
- Administration Manager
- Senior HR Officer
- Senior Manager Of Operations




 RSS Feed
RSS Feed
